Abstract
Background: Atrial fibrillation is a common arrhythmia in patients with left ventricular dysfunction associated with increased morbidity and mortality. The present study investigated the potential of dofetilide to restore and maintain sinus rhythm in patients with left ventricular dysfunction, which might reduce mortality and hospitalizations.
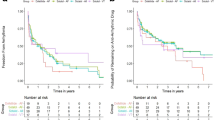
Methods and Results: In the Danish Investigations of Arrhythmia and Mortality ON Dofetilide (DIAMOND) studies, 506 patients were in atrial fibrillation (AF) or atrial flutter (AFl) at baseline. Over the course of study, cardioversion occurred in 148 (59%) dofetilide- and 86 (34%) placebo-treated patients. In these patients, the probability of maintaining sinus rhythm for 1 year was 79% with dofetilide versus 42% with placebo (P < 0.001). Dofetilide had no effect on all-cause mortality, but restoration and maintenance of sinusrhythm (independent of study treatment) was associated with a significant reduction in mortality (risk ratio [RR], 0.44; 95% CI, 0.30 to 0.64; P < 0.0001). In addition, dofetilide therapy was associated with a significantly lower risk ratio versus placebo for either all-cause (RR, 0.70; 95% CI, 0.56 to 0.89; P ≤ 0.005) or congestive heart failure (RR, 0.69; 95% CI, 0.51 to 0.93; P ≤ 0.02) rehospitalization.
Conclusions: Dofetilide is safe and increases the probability of obtaining and maintaining sinus rhythm in patients with structural heart disease. The present study suggests that restoration of sinus rhythm—on placebo or dofetilide—is associated with improved survival.
Similar content being viewed by others
References
Pritchett EL. Management of atrial fibrillation. N Engl J Med 1992;326:1264-1271.
Middlekauff HR, Stevenson WG, Stevenson LW. Prognostic significance of atrial fibrillation in advanced heart failure. A study of 390 patients. Circulation 1991;84:40-48.
Dries DL, Exner DV, Gersh BJ, Domanski MJ, Waclawiw MA, Stevenson LW. Atrial fibrillation is associated with an increased risk for mortality and heart failure progression in patients with asymptomatic and symptomatic left ventricular systolic dysfunction: A retrospective analysis of the SOLVD trials. Studies of Left Ventricular Dysfunction. J AmColl Cardiol 1998;32:695-703.
Greenbaum R CT, Channer KS, Dalrymple HW, Kingma JH, Santini M, Theisen K, Toivonnen LK. Conversion of atrial fibrillation and maintenance of sinus rhythm by dofetilide: The EMERAL (European and Australian Multicenter Evaluative Research of Atrial Fibrillation Dofetilide) study. Circulation 1998;98(Suppl 1):I-633.
Singh S, Zoble RG, Yellen L, Brodsky MA, Feld GK, Berk M, Billing CB,Jr. Efficacy and safety of oral dofetilide in converting to and maintaining sinus rhythm in patients with chronic atrial fibrillation or atrial flutter: The symptomatic atrial fibrillation investigative research on dofetilide (SAFIRE-D) study. Circulation 2000;102:2385-2390.
Torp-Pedersen C, Moller M, Bloch-Thomsen PE, Kober L, Sandoe E, Egstrup K, Agner E, Carlsen J, Videbaek J, Marchant B, Camm AJ. Dofetilide in patients with congestive heart failure and left ventricular dysfunction. Danish Investigations of Arrhythmia and Mortality on Dofetilide Study Group. N Engl J Med 1999;341:857-865.
Kober L, Bloch Thomsen PE, Moller M, Torp-Pedersen C, Carlsen J, Sandoe E, Egstrup K, Agner E, Videbaek J, Marchant B, Camm AJ. Effect of dofetilide in patients with recent myocardial infarction and left-ventricular dysfunction: A randomised trial. Lancet 2000;356:2052-2058.
Deedwania PC, Singh BN, Ellenbogen K, Fisher S, Fletcher R, Singh SN. Spontaneous conversion and maintenance of sinus rhythm by amiodarone in patients with heart failure and atrial fibrillation: Observations from the veterans affairs congestive heart failure survival trial of antiarrhythmic therapy (CHF-STAT). The Department of Veterans Affairs CHF-STAT Investigators. Circulation 1998;98:2574-2579.
Gosselink AT, Crijns HJ, Van Gelder IC, Hillige H, Wiesfeld AC, Lie KI. Low-dose amiodarone for maintenance of sinus rhythm after cardioversion of atrial fibrillation or flutter. Jama 1992;267:3289-3293.
Karlson BW, Herlitz J, Edvardsson N, Olsson SB. Prophylactic treatment after electroconversion of atrial fibrillation. Clin Cardiol 1990;13:279-286.
Levy S, Breithardt G, Campbell RW, Camm AJ, Daubert JC, Allessie M, Aliot E, Capucci A, Cosio F, Crijns H, Jordaens L, Hauer RN, Lombardi F, Luderitz B. Atrial fibrillation: Current knowledge and recommendations for management. Working Group on Arrhythmias of the European Society of Cardiology. Eur Heart J 1998;19:1294-1320.
Kieny JR, Sacrez A, Facello A, Arbogast R, Bareiss P, Roul G, Demangeat JL, Brunot B, Constantinesco A. Increase in radionuclide left ventricular ejection fraction after cardioversion of chronic atrial fibrillation in idiopathic dilated cardiomyopathy. Eur Heart J 1992;13:1290-1295.
Raymond RJ, Lee AJ, Messineo FC, Manning WJ, Silverman DI. Cardiac performance early after cardioversion from atrial fibrillation. AmHeart J 1998;136:435-442.
Wyse DG, Waldo AL, DiMarco JP, Domanski MJ, Rosenberg Y, Schron EB, Kellen JC, Greene HL, Mickel MC, Dalquist JE, Corley SD. A comparison of rate control and rhythm control in patients with atrial fibrillation. N Engl J Med 2002;347:1825-1833.
Van Gelder IC, Hagens VE, Bosker HA, Kingma JH, Kamp O, Kingma T, Said SA, Darmanata JI, Timmermans AJ, Tijssen JG, Crijns HJ. A comparison of rate control and rhythm control in patients with recurrent persistent atrial fibrillation. N Engl J Med 2002;347:1834-1840.
Rationale and design of a study assessing treatment strategies of atrial fibrillation in patients with heart failure: The Atrial Fibrillation and Congestive Heart Failure (AF-CHF) trial. Am Heart J 2002;144:597-607.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Pedersen, O.D., Brendorp, B., Elming, H. et al. Does Conversion and Prevention of Atrial Fibrillation Enhance Survival in Patients with Left Ventricular Dysfunction? Evidence from the Danish Investigations of Arrhythmia and Mortality ON Dofetilide/(DIAMOND) Study. Card Electrophysiol Rev 7, 220–224 (2003). https://doi.org/10.1023/B:CEPR.0000012386.82055.81
Issue Date:
DOI: https://doi.org/10.1023/B:CEPR.0000012386.82055.81