Abstract
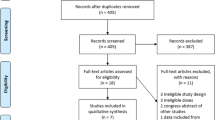
Long-term therapy with low-dose aspirin (acetylsalicylic acid; ASA), 75–325 mg, is highly effective for the secondary prevention of cardiovascular (CV) events. For high-CV-risk patients to attain the full benefits of this therapy, it is important that treatment is continuous and that good compliance is maintained over the long term. We aimed to quantify the level of, and investigate the reasons for, patient-driven non-compliance and treatment discontinuation among patients taking low-dose ASA for the prevention of CV events. We therefore performed a systematic search of the PubMed, Embase, and Cochrane databases using the terms ‘aspirin’ AND ‘patient compliance’ OR ‘withdrawal’, with no restrictions on the start date and up to July 2008. A total of 32 studies, summarizing >144 800 patients, were selected from over 400 results for inclusion. Poor compliance (defined differently among the studies included) with low-dose ASA therapy ranged from approximately 10% to over 50%, and patient-initiated discontinuation of therapy occurred in up to 30% of patients. Common predictors of both non-compliance and treatment discontinuation were lower education level, female sex, or a history of depression, diabetes mellitus, or cigarette smoking. Adverse events were cited as the reason for low-dose ASA discontinuation in almost 50% of patients. The findings of this review suggest that poor compliance is common among patients receiving low-dose ASA therapy, placing them at substantial risk of CV events. By addressing barriers to compliance with low-dose ASA therapy, healthcare professionals can improve CV risk management for such patients.










Similar content being viewed by others
References
Patrono C, Bachmann F, Baigent C, et al. Expert consensus document on the use of antiplatelet agents. The task force on the use of antiplatelet agents in patients with atherosclerotic cardiovascular disease of the European Society of Cardiology. Eur Heart J 2004 Jan; 25(2): 166–81.
Antithrombotic Trialistsś Collaboration. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ 2002 Jan 12; 324(7329): 71–86.
Harrington RA, Becker RC, Ezekowitz M, et al. Antithrombotic therapy for coronary artery disease. The Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004 Sep; 126(3 Suppl.): 513S–48S.
Patrono C, Coller B, FitzGerald GA, et al. Platelet-active drugs: the relationships among dose, effectiveness, and side effects. The Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest 2004 Sep; 126(3 Suppl.): 234S–64S.
US Preventive Services Task Force. Aspirin for the prevention of cardiovascular disease: US Preventive Services Task Force recommendation statement. Ann Intern Med 2009 Mar 17; 150(6): 396–404.
Antiplatelet Trialistsś Collaboration. Collaborative overview of randomised trials of antiplatelet therapy. I: Prevention of death, myocardial infarction, and stroke by prolonged antiplatelet therapy in various categories of patients. BMJ 1994 Jan 8; 308(6921): 81–106.
Campbell CL, Smyth S, Montalescot G, et al. Aspirin dose for the prevention of cardiovascular disease: a systematic review. JAMA 2007 May 9; 297(18): 2018–24.
Ajani UA, Ford ES, Greenland KJ, et al. Aspirin use among U.S. adults: behavioral risk factor surveillance system. Am J Prev Med 2006 Jan; 30(1): 74–7.
Chen WH, Cheng X, Lee PY, et al. Aspirin resistance and adverse clinical events in patients with coronary artery disease. Am J Med 2007 Jul; 120(7): 631–5.
Krasopoulos G, Brister SJ, Beattie WS, et al. Aspirin “resistance” and risk of cardiovascular morbidity: systematic review and meta-analysis. BMJ 2008 Jan 26; 336(7637): 195–8.
Hanjis C, Frishman WH, Lerner RG. Aspirin resistance: mechanisms and clinical implications. Cardiol Rev 2006 Jan-Feb; 14(1): 18–25.
Biondi-Zoccai GG, Lotrionte M, Agostoni P, et al. A systematic review and meta-analysis on the hazards of discontinuing or not adhering to aspirin among 50,279 patients at risk for coronary artery disease. Eur Heart J 2006 Nov; 27(22): 2667–74.
Eagle KA, Kline-Rogers E, Goodman SG, et al. Adherence to evidence-based therapies after discharge for acute coronary syndromes: an ongoing prospective, observational study. Am J Med 2004 Jul 15; 117(2): 73–81.
Kulkarni SP, Alexander KP, Lytle B, et al. Long-term adherence with cardiovascular drug regimens. Am Heart J 2006 Jan; 151(1): 185–91.
Sappok T, Faulstich A, Stuckert E, et al. Compliance with secondary prevention of ischemic stroke: aprospective evaluation. Stroke 2001 Aug; 32(8): 1884–9.
Simpson E, Beck C, Richard H, et al. Drug prescriptions after acute myocardial infarction: dosage, compliance, and persistence. Am Heart J 2003 Mar; 145(3): 438–44.
Sud A, Kline-Rogers EM, Eagle KA, et al. Adherence to medications by patients after acute coronary syndromes. Ann Pharmacother 2005 Nov; 39(11): 1792–7.
Wald DS, Morton G, Walker K, et al. Long-term continuation on cardiovascular drug treatment in patients with coronary heart disease. Ann Pharmacother 2007 Oct; 41(10): 1644–7.
Bachman DS. Discontinuing chronic aspirin therapy: another risk factor for stroke? Ann Neurol 2002 Jan; 51(1): 137–8.
Collet JP, Himbet F, Steg PG. Myocardial infarction after aspirin cessation in stable coronary artery disease patients. Int J Cardiol 2000 Nov–Dec; 76(2–3): 257–8.
McFadden EP, Stabile E, Regar E, et al. Late thrombosis in drug-eluting coronary stents after discontinuation of antiplatelet therapy. Lancet 2004 Oct 23–29; 364(9444): 1519–21.
Mitchell SM, Sethia KK. Hazards of aspirin withdrawal before transurethral prostatectomy. BJU Int 1999 Sep; 84(4): 530.
Ferrari E, Benhamou M, Cerboni P, et al. Coronary syndromes following aspirin withdrawal: a special risk for late stent thrombosis. J Am Coll Cardiol 2005 Feb 1; 45(3): 456–9.
Ho PM, Spertus JA, Masoudi FA, et al. Impact of medication therapy discontinuation on mortality after myocardial infarction. Arch Intern Med 2006 Sep 25; 166(17): 1842–7.
Newby LK, LaPointe NM, Chen AY, et al. Long-term adherence to evidencebased secondary prevention therapies in coronary artery disease. Circulation 2006 Jan 17; 113(2): 203–12.
Carney RM, Freedland KE, Eisen SA, et al. Major depression and medication adherence in elderly patients with coronary artery disease. Health Psychol 1995 Jan; 14(1): 88–90.
Carney RM, Freedland KE, Eisen SA, et al. Adherence to a prophylactic medication regimen in patients with symptomatic versus asymptomatic ischemic heart disease. Behav Med 1998 Spring; 24(1): 35–9.
De Schryver EL, van Gijn J, Kappelle LJ, et al. Non-adherence to aspirin or oral anticoagulants in secondary prevention after ischaemic stroke. J Neurol 2005 Nov; 252(11): 1316–21.
Silagy CA, McNeil JJ, Donnan GA, et al. The PACE pilot study: 12-month results and implications for future primary prevention trials in the elderly (Prevention with low-dose Aspirin of Cardiovascular disease in the Elderly). J Am Geriatr Soc 1994 Jun; 42(6): 643–7.
Hamann GF, Weimar C, Glahn J, et al. Adherence to secondary stroke prevention strategies: results from the German Stroke Data Bank. Cerebrovasc Dis 2003; 15(4): 282–8.
Komiya T, Kudo M, Urabe T, et al. Compliance with antiplatelet therapy in patients with ischemic cerebrovascular disease: assessment by platelet aggregation testing. Stroke 1994 Dec; 25(12): 2337–42.
Mant J, Hobbs FD, Fletcher K, et al. Warfarin versus aspirin for stroke prevention in an elderly community population with atrial fibrillation (the Birmingham Atrial Fibrillation Treatment of the Aged Study, BAFTA): a randomised controlled trial. Lancet 2007 Aug 11; 370(9586): 493–503.
Morant SV, McMahon AD, Cleland JG, et al. Cardiovascular prophylaxis with aspirin: costs of supply and management of upper gastrointestinal and renal toxicity. Br J Clin Pharmacol 2004 Feb; 57(2): 188–98.
Rieckmann N, Kronish IM, Haas D, et al. Persistent depressive symptoms lower aspirin adherence after acute coronary syndromes. Am Heart J 2006 Nov; 152(5): 922–7.
Waeber B, Leonetti G, Kolloch R, et al. Compliance with aspirin or placebo in the Hypertension Optimal Treatment (HOT) study. J Hypertens 1999 Jul; 17(7): 1041–5.
Wang Y, Wu D, Ma R, et al. A survey on adherence to secondary ischemic stroke prevention. Neurol Res 2006 Jan; 28(1): 16–20.
Califf RM, DeLong ER, Ostbye T, et al. Underuse of aspirin in a referral population with documented coronary artery disease. Am J Cardiol 2002 Mar 15; 89(6): 653–61.
Collet JP, Montalescot G, Blanchet B, et al. Impact of prior use or recent withdrawal of oral antiplatelet agents on acute coronary syndromes. Circulation 2004 Oct 19; 110(16): 2361–7.
Matsuzaki K, Matsui K, Haraguchi N, et al. Ischemic heart attacks following cessation of aspirin before coronary artery bypass surgery: a report of two cases. Ann Thorac Cardiovasc Surg 1999 Apr; 5(2): 121–2.
Newby LK, Bhapkar MV, White HD, et al. Aspirin use post-acute coronary syndromes: intolerance, bleeding and discontinuation. J Thromb Thrombolysis 2003 Dec; 16(3): 119–28.
Sibon I, Orgogozo JM. Antiplatelet drug discontinuation is a risk factor for ischemic stroke. Neurology 2004 Apr 13; 62(7): 1187–9.
Cotter G, Shemesh E, Zehavi M, et al. Lack of aspirin effect: aspirin resistance or resistance to taking aspirin? Am Heart J 2004 Feb; 147(2): 293–300.
Glynn RJ, Buring JE, Manson JE, et al. Adherence to aspirin in the prevention of myocardial infarction: The Physiciansś Health Study. Arch Intern Med 1994 Dec 12–26; 154(23): 2649–57.
Maulaz AB, Bezerra DC, Michel P, et al. Effect of discontinuing aspirin therapy on the risk of brain ischemic stroke. Arch Neurol 2005 Aug; 62(8): 1217–20.
Derry S, Loke YK. Risk of gastrointestinal haemorrhage with long term use of aspirin: meta-analysis. BMJ 2000 Nov 11; 321(7270): 1183–7.
Serrano P, Lanas A, Arroyo MT, et al. Risk of upper gastrointestinal bleeding in patients taking low-dose aspirin for the prevention of cardiovascular diseases. Aliment Pharmacol Ther 2002 Nov; 16(11): 1945–53.
Sorensen HT, Mellemkjaer L, Blot WJ, et al. Risk of upper gastrointestinal bleeding associated with use of low-dose aspirin. Am J Gastroenterol 2000 Sep; 95(9): 2218–24.
Weil J, Colin-Jones D, Langman M, et al. Prophylactic aspirin and risk of peptic ulcer bleeding. BMJ 1995 Apr 1; 310(6983): 827–30.
Simmons DL, Botting RM, Hla T. Cyclooxygenase isozymes: the biology of prostaglandin synthesis and inhibition. Pharmacol Rev 2004 Sep; 56(3): 387–437.
Laine L, Takeuchi K, Tarnawski A. Gastric mucosal defense and cytoprotection: bench to bedside. Gastroenterology 2008 Jul; 135(1): 41–60.
Norman M, Parker MJ. Compliance with a pharmacological secondary fracture prevention policy. Injury 2006 Aug; 37(8): 718–20.
ten Doesschate MC, Koeter MW, Bockting CL, et al. Health related quality of life in recurrent depression: a comparison with a general population sample. J Affect Disord 2010 Jan; 120(1–3): 126–32.
Adams AS, Trinacty CM, Zhang F, et al. Medication adherence and racial differences in A1C control. Diabetes Care 2008 May; 31(5): 916–21.
Walker EA, Molitch M, Kramer MK, et al. Adherence to preventive medications: predictors and outcomes in the Diabetes Prevention Program. Diabetes Care 2006 Sep; 29(9): 1997–2002.
Bonolo P, César C, Acúrcio F, et al. Non-adherence among patients initiating antiretroviral therapy: a challenge for health professionals in Brazil. AIDS 2005; 19 Suppl. 4: S5–13.
Diaz-Fuentes G, Rodriguez J, Maluf C, et al. Improving compliance for prophylaxis of venous thromboembolism. Internet J Intern Med 2006; 6 (1).
Fredericks EM, Magee JC, Opipari-Arrigan L, et al. Adherence and healthrelated quality of life in adolescent liver transplant recipients. Pediatr Transplant 2008 May; 12(3): 289–99.
Burger W, Chemnitius JM, Kneissl GD, et al. Low-dose aspirin for secondary cardiovascular prevention-cardiovascular risks after its perioperative withdrawal versus bleeding risks with its continuation-review and metaanalysis. J Intern Med 2005 May; 257(5): 399–414.
Beving H, Zhao C, Albage A, et al. Abnormally high platelet activity after discontinuation of acetylsalicylic acid treatment. Blood Coagul Fibrinolysis 1996 Jan; 7(1): 80–4.
Mousa SA, Forsythe MS, Bozarth JM, et al. Effect of single oral dose of aspirin on human platelet functions and plasma plasminogen activator inhibitor-1. Cardiology 1993; 83(5–6): 367–73.
Coleman JL, Alberts MJ. Effect of aspirin dose, preparation, and withdrawal on platelet response in normal volunteers. Am J Cardiol 2006 Sep 15; 98(6): 838–41.
Serebruany VL, Malinin AI, Bhatt DL. Paradoxical rebound platelet activation after painkillers cessation: missing risk for vascular events? Am J Med 2006 Aug; 119(8): 707 e1 1–6.
Chiang N, Bermudez EA, Ridker PM, et al. Aspirin triggers antiinflammatory 15-epi-lipoxin A4 and inhibits thromboxane in a randomized human trial. Proc Natl Acad Sci U S A 2004 Oct 19; 101(42): 15178–83.
Aguejouf O, Eizayaga F, Desplat V, et al. Prothrombotic and hemorrhagic effects of aspirin. Clin Appl Thromb Hemost 2009 Oct; 15(5): 523–8.
Kroenke K, Pinholt EM. Reducing polypharmacy in the elderly: a controlled trial of physician feedback. J Am Geriatr Soc 1990 Jan; 38(1): 31–6.
CAPRIE Steering Committee. A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). Lancet 1996 Nov 16; 348(9038): 1329–39.
Laheij RJ, Jansen JB, Verbeek AL, et al. Helicobacter pylori infection as a risk factor for gastrointestinal symptoms in patients using aspirin to prevent ischaemic heart disease. Aliment Pharmacol Ther 2001 Jul; 15(7): 1055–9.
Garcia Rodriguez LA, Hernandez-Diaz S. Risk of uncomplicated peptic ulcer among users of aspirin and nonaspirin nonsteroidal antiinflammatory drugs. Am J Epidemiol 2004 Jan 1; 159(1): 23–31.
Yeomans ND, Lanas AI, Talley NJ, et al. Prevalence and incidence of gastroduodenal ulcers during treatment with vascular protective doses of aspirin. Aliment Pharmacol Ther 2005 Nov 1; 22(9): 795–801.
Chisholm-Burns MA, Spivey CA. Pharmacoadherence: a new term for a significant problem. Am J Health Syst Pharm 2008 Apr 1; 65(7): 661–7.
Diaz-Fuentes G, Rodriguez J, Maluf C, et al. Improving compliance for prophylaxis of venous thromboembolism. Internet J Intern Med 2006; 6 (1).
Gallefoss F, Bakke PS. How does patient education and self-management among asthmatics and patients with chronic obstructive pulmonary disease affect medication? Am J Respir Crit Care Med 1999 Dec; 160(6): 2000–5.
Kripalani S, Yao X, Haynes RB. Interventions to enhance medication adherence in chronic medical conditions: a systematic review. Arch Intern Med 2007 Mar 26; 167(6): 540–50.
van Dulmen S, Sluijs E, van Dijk L, et al. Patient adherence to medical treatment: a review of reviews. BMC Health Serv Res 2007; 7: 55.
Patrono C, Garcia Rodriguez LA, Landolfi R, et al. Low-dose aspirin for the prevention of atherothrombosis. N Engl J Med 2005 Dec 1; 353(22): 2373–83.
Lanas A, Scheiman J. Low-dose aspirin and upper gastrointestinal damage: epidemiology, prevention and treatment. Curr Med Res Opin 2007 Jan; 23(1): 163–73.
Yeomans N, Lanas A, Labenz J, et al. Efficacy of esomeprazole (20mg once daily) for reducing the risk of gastroduodenal ulcers associated with continuous use of low-dose aspirin. Am J Gastroenterol 2008 Oct; 103(10): 2465–73.
Kahrilas PJ, Shaheen NJ, Vaezi MF, et al. American Gastroenterological Association Medical Position Statement on the management of gastroesophageal reflux disease. Gastroenterology 2008 Oct; 135(4): 1383–91, 91 e1–5.
Pezalla E, Day D, Pulliadath I. Initial assessment of clinical impact of a drug interaction between clopidogrel and proton pump inhibitors. J Am Coll Cardiol 2008 Sep 16; 52(12): 1038–9; author reply: 1039.
Juurlink DN, Gomes T, Ko DT, et al. A population-based study of the drug interaction between proton pump inhibitors and clopidogrel. CMAJ 2009 Mar 31; 180(7): 713–8.
Simon T, Verstuyft C, Mary-Krause M, et al. Genetic determinants of response to clopidogrel and cardiovascular events. N Engl J Med 2009 Jan 22; 360(4): 363–75.
Gilard M, Arnaud B, Cornily JC, et al. Influence of omeprazole on the antiplatelet action of clopidogrel associated with aspirin: the randomized, doubleblind OCLA (Omeprazole CLopidogrel Aspirin) study. J Am Coll Cardiol 2008 Jan 22; 51(3): 256–60.
Aubert RE, Epstein RS, Teagarden JR, et al. Proton pump inhibitors effect on clopidogrel effectiveness: the clopidogrel Medco outcomes study [abstract]. Circulation 2008; 118(18): S815.
Dunn SP, Macaulay TE, Brennan DM, et al. Baseline proton pump inhibitor use is associated with increased cardiovascular events with and without the use of clopidogrel in the CREDO trial [abstract]. Circulation 2008; 118(18): S815.
Zairis M, Patsourakos N, Makrygiannis S, et al. The impact of oral proton pump inhibitors on the effectiveness of combined aspirin and clopidogrel drug therapy during the first year after elective coronary stenting [abstract]. Eur Heart J 2008; 29 Suppl.: 134.
Ramirez JF, Selzer F, Chakaprani R, et al. Proton pump inhibitor and clopidogrel combination is not associated with adverse clinical outcomes after PCI: the NHLBI dynamic registry [abstract]. J Am Coll Cardiol 2009; 53(10 Suppl. 1): 2903.
O’Donoghue ML, Braunwald E, Antman EM, et al. Pharmacodynamic effect and clinical efficacy of clopidogrel and prasugrel with or without a protonpump inhibitor: an analysis of two randomised trials. Lancet 2009 Sep 19; 374(9694): 989–97.
Muldowney J, Benge CD. Combination therapy with clopidogrel and protonpump inhibitors [letter]. Lancet 2010; 375: 27.
Bhala N, Banerjee A. Combination therapy with clopidogrel and proton-pump inhibitors [letter]. Lancet 2010; 375(9708): 28; author reply: 28–9.
Dezii CM. A retrospective study of persistence with single-pill combination therapy vs. concurrent two-pill therapy in patients with hypertension. Manag Care 2000 Sep; 9(9 Suppl.): 2–6.
Sapienza S, Sacco P, Floyd K, et al. Results of a pilot pharmacotherapy quality improvement program using fixed-dose, combination amlodipine/benazepril antihypertensive therapy in a long-term care setting. Clin Ther 2003 Jun; 25(6): 1872–87.
Bangalore S, Kamalakkannan G, Parkar S, et al. Fixed-dose combinations improve medication compliance: a meta-analysis. Am J Med 2007 Aug; 120(8): 713–9.
Acknowledgments
This review was supported by AstraZeneca, the manufacturers of esomeprazole. We thank Claire Byrne and Anna Mett, from Wolters Kluwer, who provided medical writing support funded by AstraZeneca. Dr Tóth is a member of the speaker’s bureau and is a consultant for AstraZeneca. Dr Næsdal is an employee of AstraZeneca. Dr Herlitz has no conflicts of interest that are relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Herlitz, J., Tóth, P.P. & Næsdal, J. Low-Dose Aspirin Therapy for Cardiovascular Prevention. Am J Cardiovasc Drugs 10, 125–141 (2010). https://doi.org/10.2165/11318440-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11318440-000000000-00000