Article Text
Abstract
Background National guidance for England recommends that cardiovascular disease (CVD) should be managed as a family of diseases in the community. Here, we describe the results of such an approach.
Methods Patients with established CVD or who were at high multifactorial risk (HRI) underwent a 12-week community-based nurse-led prevention programme (MyAction) that included lifestyle and risk factor management, prescription of medication and weekly exercise and education sessions.
Results Over a 6-year period, 3232 patients attended an initial assessment; 63% were male, and 48% belonged to black and minority ethnic groups. 56% attended an end-of-programme assessment, and 33% attended a one year assessment. By the end of the programme, there was a significant reduction in smoking prevalence but only in HRI (−3.7%, p<0.001). Mediterranean diet score increased in both CVD (+1.2, p<0.001) and HRI (+1.5; p<0.001), as did fitness levels (CVD +0.8 estimated Mets maximum, p<0.001, HRI +0.9 estimated Mets maximum, p<0.001) and the proportions achieving their physical activity targets (CVD +40%, p<0.001, HRI +37%, p<0.001). There were significant increases in proportions achieving their blood pressure (CVD +15.4%, p<0.001, HRI +25%, p<0.001 and low-density lipoprotein cholesterol targets (CVD +6%, p=0.004, HRI +23%, p<0.001). Statins and antihypertensive medications significantly increased in HRI. Significant improvements in depression scores and quality-of-life measures were also seen. The majority of improvements were maintained at 1 year.
Conclusion These results demonstrate that an integrated vascular prevention programme is feasible in practice and reduces cardiovascular risk in patients with established CVD and in those at high multifactorial risk.
- Cardiovascular disease prevention
- lifestyle
- cardiovascular risk factors
- rehabilitation
- integrated care
This is an Open Access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
Statistics from Altmetric.com
Background
Recently published guidance on improving cardiovascular disease (CVD) outcomes in England states that CVD is a single family of diseases and should be managed in an integrated manner.1 However, acute coronary syndromes, transient ischaemic attack, stroke and claudication are typically managed in silos of care through cardiology, stroke and vascular services. While such a disease-specific approach may be appropriate for acute treatment, it is less so for prevention, as the risk factors for CVD are overarching, and many patients have vascular disease in more than one territory (i.e. polyvascular disease).2 Despite the paradigm shift to total cardiovascular risk, this silo approach is even more evident for risk factors for CVD, for example, specialist clinics for hypertension, hypercholesterolaemia and diabetes mellitus. Nevertheless, all these patients require the same comprehensive lifestyle intervention, risk factor and therapeutic management to reduce their risk of disease progression, hospitalisations and revascularisation and also to improve life expectancy.3 4
In 2008, we published the results of a cluster randomised controlled trial of a nurse-coordinated multidisciplinary, family-based cardiovascular disease prevention programme (EUROACTION) that was conducted in hospital and general practice across eight European countries.5 The programme used a behavioural approach to address lifestyle together with medical risk factor management and the use of cardioprotective medications. At 1 year, the programme demonstrated healthier lifestyle changes and improvements in other risk factors for patients with coronary heart disease and those at high risk of CVD and their partners than those in usual care.
We subsequently integrated secondary and primary prevention into one community-based CVD prevention programme, which we called MyAction (figure 1). We piloted the feasibility of this approach in a public leisure facility in the National Health Service (NHS) and demonstrated that it achieved the same, or even better, short-term outcomes as the EUROACTION trial,6 although the population in which it was conducted was principally white and relatively affluent.
The MyAction prevention programme.
In 2009, a programme of systematic assessment of total cardiovascular risk (Health Checks) began in primary care in England on all those aged 40–74 years. Concurrently, Imperial College Healthcare NHS Trust was commissioned by Public Health in Westminster, London to deliver the MyAction programme as a risk management programme for those identified through the Health Checks. Westminster is culturally and socioeconomically diverse, ranking 75th most deprived out of 354 local authorities, and over 30% of the population belong to black and minority ethnic (BME) groups. Here, we describe the clinical and patient reported outcomes of the programme in this population.
Methods
The MyAction programme (figure 1) was conducted in three community hubs, each containing a multidisciplinary team (MDT): cardiovascular nurses, dietitians, physical activity specialists and administrative staff supported centrally by a lead nurse, clinical psychologist and consultant cardiologist. The MDT received training by members of the original EUROACTION team, supported by a dedicated health professional manual, patient education packs and a patient record card (see online supplementary material). Eligible patients included those at high multifactorial risk (HRI; QRisk2 >20%), those with chronic kidney disease or diabetes mellitus or those with any manifestation of coronary heart disease, peripheral arterial disease or transient ischaemic attack/minor stroke. Links with primary care were forged through stakeholder meetings, presentations at primary care forums and visits to the individual practices by the MDT. Patients were referred from primary and secondary care and contacted in person and in writing by the referral coordinator. Interpreting services and transport services were offered routinely.
At the initial assessment (IA) by the MDT, the following parameters were assessed: smoking habit self–report and breath carbon monoxide; dietary habits, including diet history, a food habit questionnaire and adherence to the Mediterranean diet score (using a dietician-administered 14-item adherence tool available at http://www.unav.es/preventiva/predimed/pagina10.html)7 as well as use of and adherence to cardioprotective medications. The following measurements were made using standardised instruments: weight and height, body mass index (BMI) and waist circumference; physical activity levels (7-day physical activity recall that includes an intensity domain),8 functional capacity (Chester Step Test)9 and blood pressure (BP). Laboratory testing included a full lipid profile, liver, thyroid and renal function and HbA1c. Patient-reported outcome measures were also assessed, including the dimension-specific Hospital Anxiety and Depression Scale,10 the EuroQol Visual Analogue Scale11 and the Dartmouth COOP, which consists of nine items measuring all domains of health-related quality of life.12
The MDT also identified the patients’ priorities in terms of reducing their cardiovascular risk, as well as exploring beliefs, barriers and motivators to change. Motivational interviewing and goal setting were key behaviour change strategies used. The 12-week programme included individualised follow-up, a weekly educational workshop and supervised exercise session with only simple equipment in order to give patients the confidence to become physically active in their everyday lives. A weekly meeting held between the MDT and cardiologist enabled review of cardiovascular risk factor management, including medication (uptitrating doses for beta blockers and ACE inhibitors/angiotensin receptor blockers (ARBs) to the doses used in clinical trials and adding new drugs) as appropriate. Therapeutic decisions were communicated to the primary care practitioner. The BP target was <140/90 mm Hg. The total cholesterol target was <5 mmol/L and <4 mmol/L and the LDL-cholesterol target was <3 and 2 mmol/L for patients with HRI and CVD respectively. After programme completion, the patients underwent an end-of-programme (EOP) assessment with a further assessment at 1 year.
Statistical analyses
Continuous variables were summarised using means and standard deviations or medians and interquartile ranges, while percentages were used to summarise binary variables. The unpaired t-test (or Mann-Whitney U test) were used to compare continuous variables between those who attended EOP with those who did not. The x² test (or Fisher’s exact test) was used for similar comparisons of categorical variables.
The change in outcomes between IA and EOP and IA and one year were evaluated for those who had measurements on both occasions. Continuous outcomes were analysed using the paired t-test or the Wilcoxon matched-pairs test, while McNemar’s test was used for categorical outcomes. Confidence intervals for differences in means, medians or percentages were calculated. All significance tests were performed at the 5% level. The statistical package used was Stata version 13.1.
Results
Programme activity and adherence
A flow chart of programme activity is provided in figure 2. Between June 2009 and 2015, 5103 referrals were received, and 3232 (63%) patients attended an IA. Of these patients, 50.8% were asymptomatic and mostly at high risk; 39.5% had vascular disease, mostly coronary artery disease and 7.1% were referred with a diagnosis of diabetes. Table 1 describes their characteristics at the IA. 63.4% were men, and the mean (SD) age was 63.5 (10.7) years. 48% were white, and South Asian, Arabic and Afro Caribbean were the most common other ethnicities. 92.2% of those assessed agreed to participate in the programme and participation rates were similar across all the principal ethnic groups (see online supplementary table S1). Mean (SD) attendance rates were: 5.9 (5.2) education sessions and 6.8 (5.7) exercise sessions attended (out of a total of 12). 1521 (55.9%) attended an EOP assessment and 32.9% had follow-up at 1 year. Patient characteristics at the IA, which predicted those less likely to attend an EOP assessment, included younger age, male gender, non-white ethnicity, history of CVD, current smoking, less optimal diet and physical activity levels, lower education levels, higher baseline anxiety and depression and lower quality of life scores (see online supplementary table S2).
Activity overview.
Characteristics of those who attended the initial assessment (IA)
Clinical outcomes
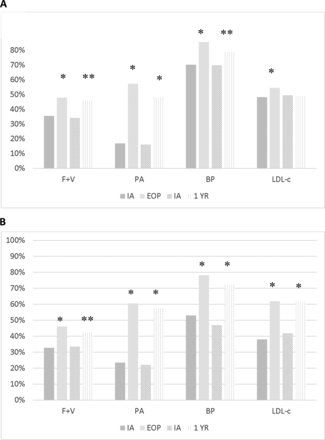
Tables 2 and 3 present results on changes in lifestyle, medical risk factors, cardioprotective medications and patient-reported outcome measures between IA and EOP and between IA and 1 year for patients with CVD and HRI respectively. The comparison is based on the same patients attending at both time points. Figure 3A, B illustrate the proportions achieving targets for fruit and vegetables, physical activity, BP and LDL-cholesterol for both groups at both time points.
Proportions of patients with CVD (A) and high-risk individuals (B) achieving targets for fruits and vegetables, physical activity, BP and LDL-c.
Targets: fruits and vegetables >5 portions/day; physical activity ≥5 times/week ≥30 min; BP <140/90 mm Hg; LDL-c <3 for HRI and <2 mmol/L for CVD and diabetes mellitus, *p<0.001, **p<0.005. BP, blood pressure; CVD, cardiovascular disease; HRI, high multifactorial risk; LDL-c, low-density lipoprotein cholesterol;
Changes (mean change or change in proportion followed by 95% CI) in lifestyle, medical risk factors, cardioprotective medication and patient-reported outcome measures in cardiovascular patients between the IA, EOP and 1-year assessments
Changes (mean change or change in proportion followed by 95% CI) in lifestyle, medical risk factors, cardioprotective medication and patient-reported outcome measures in high-risk individuals between the IA, EOP and 1-year assessments
Lifestyle
Smoking
In HRI, a significant absolute quit rate was seen by EOP, but this was not significant at 1 year, and there were no significant change in smoking habits in patients with CVD, although 40% of them reported making at least one quit attempt. The use of nicotine replacement therapy (NRT) was high in both groups where quit attempts were made (62.5% and 60% for CVD and HRI, respectively), but the use of varenicline therapy was low (0% in CVD patients and 10% in HRI).
Diet
In both patients with HRI and CVD, there were significant improvements in fruit and vegetable consumption, fish consumption and adherence to a cardioprotective diet, as measured by the Mediterranean diet score at EOP, and these improvements were maintained at 1 year in both groups.
Physical activity
Only 1 in 5 patients were achieving their physical activity targets at baseline, but this increased to about 1 in 2 by EOP in both groups, with this improvement again being maintained at 1 year. Cardiorespiratory fitness (estimated Mets max) also improved significantly in both groups at both time points.
Anthropometry
Significant reductions were seen in weight (HRI) and waist circumference (CVD and HRI), and these changes were maintained at 1 year.
Medical risk factors and cardioprotective medication
Significant increases in proportions achieving their BP and lipid targets were seen in both patient groups at EOP and 1 year, but for lipids, this improvement was significant at 1 year in HRI only. Only a small percentage of patients were newly diagnosed with diabetes at the IA (all patients had HbA1c at baseline). There were no improvements in HbA1c in those with known diabetes or newly diagnosed at the IA.
In patients with CVD, the baseline use of cardioprotective medication was high, but there was an increased use of ACE inhibitors/ARB and calcium channel blocker (CCB) by EOP, although this was not evident at 1 year. However, the emphasis of the programme was on adherence and also medication up-titration to evidence-based doses, and there were significant increases in mean doses of bisoprolol (+0.4 mg; 95% CI 0.2 to 0.5) and ramipril (+1.1 mg; 95% CI 0.8 to 1.4) over the course of the programme. In HRI, however, there were significant increases in the use of statins, ACE inhibitors/ARBs, CCBs and diuretics by EOP, with these changes being maintained at 1 year.
Patient reported outcome measures
Significant reductions in depression (HRI and CVD) levels were seen by EOP, which were sustained at 1 year. There was also evidence of significant improvement in quality of life in both groups at both time points.
Discussion
The MyAction Westminster programme successfully recruited the majority of patients referred. There was evidence of healthy lifestyle changes in both primary prevention and secondary prevention patients, particularly in adherence to a cardioprotective diet and increased levels of physical fitness, maintained over the longer term. The evidence for the protective effects of a Mediterranean diet and regular physical activity in both primary and secondary prevention is well established, even if improvement occurs relatively late in life.13 14 Significant quit rates were seen for smoking in patients with HRI but not in patients with CVD, despite the programme’s nurses being trained in smoking cessation.15 However, it is well recognised that the majority of smokers stop at the time of their CVD event, and those who continue to smoke represent a more challenging addicted group.16 NRT was the most frequent drug prescribed for smoking cessation, but the use of varenicline, probably the most effective drug available for smoking cessation,17 was very low overall. In our EUROACTION Plus Varenicline trial we achieved a smoking cessation rate of 51% with a combination of a behavioural approach and varenicline in those willing to make a quit attempt, suggesting that such an integrated behavioural/pharmacotherapy approach in this population is effective.18
There were no improvements in weight among the patients with CVD who were overweight at the IA, and while there were significant reductions in central obesity (waist circumference) that were sustained at 1 year, these changes were very modest. Patients with HRI, who were a more obese group at baseline and who reported greater dietary improvements, demonstrated significant and sustained reductions in both their weight and waist circumference, which will have favourable cardiometabolic benefits.
Medical risk factors (BP and lipids) improved significantly in both patient groups, likely due to a combination of healthy lifestyle changes and the prescription of, and adherence with, cardioprotective medications. The use of medication in patients with CVD was high at the IA, reflecting good prescribing practices in secondary care, and there were further small increases in ACE/ARB and CCB over the course of the programme. More importantly, there was also up-titration in doses of ARBS/ACE and beta blockers. In HRI, there was a significant increase in use of lipid-lowering drugs and antihypertensives, which was maintained in the longer term. Although medication use was based on self-report with inherent limitations,19 the sustained improvement in BP and lipids supports these self-reported data, which is in contrast to the substantially lower levels of adherence20 to cardiovascular medications in general, so the programme was particularly successful in this respect.
Patients were actively screened for diabetes mellitus at all assessments (HbA1c), and surprisingly, only a small proportion of patients were diagnosed with new diabetes. Use of the oral glucose tolerance test would potentially have detected more patients with dysglycaemia, as well as new diabetes, but is less practical to perform in daily clinical practice.21 In addition, a proportion of high-risk individuals referred via the NHS Health Checks pathway would have already had such a screen in primary care. There was no significant change in glycaemic control in those with diabetes mellitus in both CVD and HRI, but these analyses were limited by statistical power because of small numbers.
Improvements were also seen in patient-reported outcomes with reduction in depression among both HRI and CVD, which is important, given that depression is an independent risk factor for cardiac mortality.22 Quality of life is another prime indicator of health outcome among cardiovascular patients,23 and improvements were found for both groups, which were sustained in the longer term.
The MyAction intervention was successful in engaging BME groups (about half of all participants in the programme), which is notable, as there is a paucity of evidence for successful interventions to reduce CVD risk in these groups.24 Successful factors likely included the location of the programme in two of the borough’s most deprived wards (where there is a relatively high population of BME groups), the individualised tailored approach and an emphasis on culturally appropriate advice, particularly in verbal form, with interpreters provided, as necessary. We will be reporting outcomes by ethnic group in a separate paper.
The MyAction programme therefore offers a unique approach to prevention through integration of secondary and primary prevention in a community programme, which achieved an overall reduction in cardiovascular risk for both cardiovascular patients and asymptomatic high-risk individuals, and this was sustained to 1 year. It has now been run successfully in the NHS in two different locations,6 as well as in the Republic of Ireland, broadening its evidence base.25 Recently, it has been suggested that the NHS Health Checks are not an effective use of resources, with very modest improvements in cardiovascular risk26 at a median follow-up of 2 years. We would argue that it is not the NHS Check itself that is ineffective but, rather, the lack of an integrated risk management programme for the individual who has been identified. Currently, such patients are managed in primary care by sign posting to services in the community (eg, smoking cessation services, weight management programmes, exercise on prescription, etc). Lifestyle programmes are a notable example, as many local councils (where public health now sits) are commissioning the same using health trainers despite a lack of evidence for such an approach.27 28 All these services are less likely to achieve the lifestyle and risk factor outcomes required to reduce total CVD risk than an integrated multidisciplinary programme involving nurses, dieticians and physical activity specialists. We would argue that this also holds for cardiac rehabilitation programmes in the UK29. Although recent guidelines4 for cardiac rehabilitation place equal emphasis on all aspects of secondary prevention, including lifestyle and medical risk factor management, access by programmes to physicians is limited, and audit of lipid and BP targets are hampered by a paucity of data, while there are no data available on medication use/dosage.30 The MyAction programme, on the other hand, demonstrates how a modern CVD prevention programme can deliver on all the key recommendations of the recent guidelines.
Cost: The cost of the MyAction programme intervention was approximately £1152 per patient. A full health economics assessment has been carried out and will be reported separately.
Limitations
Similar to the previously published results of the MyAction pilot, this is also a descriptive study with no control group. Some of the results may therefore be due to regression to the mean and not necessarily the effect of the MyAction programme. Nonetheless, the results are similar, or better, than those achieved in the original EUROACTION randomised controlled trial. A substantial proportion of those who attended IA did not come back for the EOP assessment or at 1 year, which is also a potential source of bias (ie, those who attended were more likely to have healthier behaviours and be more compliant with medications), making the programme appear more effective than the reality. Patients leaving such programmes is common to all cardiac rehabilitation services, and in the most recent NACR report, EOP assessment data were available on only 53% of participants. The statistical comparisons on changes over time had to be based on the same patients attending the IA and EOP and, similarly, those attending the IA and again at 1 year; otherwise, the results would be biased in favour of the programme.
Conclusion
The MyAction programme successfully recruited and retained a broad spectrum of cardiovascular and high risk patients. A nurse-led, multidisciplinary approach resulted in favourable changes in lifestyle and medical risk factors, the prescription of cardioprotective medication and improvements in patient reported outcome measures. As stated in the strategy for CVD prevention for England, a ‘more coordinated and integrated approach is needed for assessment, treatment and care to improve outcomes’.1 The MyAction model is a unique approach that manages CVD as a single family of diseases in the community and now has strong evidence for sustained clinical effectiveness in an ethnically and socioeconomically diverse population.
Postscript
In 2015, clinical commissioning groups commissioned a prevention and rehabilitation service for coronary patients (provided by Imperial College Healthcare NHS Trust), while Public Health Westminster separately commissioned a primary prevention service. Imperial College Healthcare NHS Trust was unsuccessful in its bid to continue to provide the primary-prevention service, and a private company was awarded the contract. Thus, the integrated MyAction Westminster programme was decommissioned on 30 September 30 2015.
Key messages
What is already known about this subject?
Primary and secondary prevention measures are important for reducing cardiovascular risk, but significant gaps exist between what is recommended in guidelines and what happens in daily clinical practice.
What does this study add?
Integrated preventive care across the spectrum of cardiovascular risk from those with established cardiovascular disease (coronary heart disease, peripheral arterial disease or transient ischaemic attack/minor stroke) to those with high multifactorial risk is feasible and effective in everyday clinical practice and has the potential to bridge this treatment gap.
How might this impact on clinical practice?
One of the key recommendations of the Cardiovascular Disease Outcomes Strategy for England was managing cardiovascular disease as a family of diseases in the community. This community-based programme embodies this key recommendation, and its clinical effectiveness supports such an approach on a more widespread scale.
Supplemental material
Acknowledgments
Public Health Team Westminster: AB, Dr Anna Cox, Mary Cullen. MyAction Westminster Team: Clinical Lead SBC, Consultant Cardiologist KK, Nurse Leads Sarah Jane Clements and Judith Edwards, NHS Manager Christine Yates, IT Managers Peter McCartney and Sebastien Trudgian, Nurses Tracey Hughes, Elisabeth Visagie, Gill Cowling, Mary Fry, Maria Matthews, Teresa Mackay, Tereska Siwicka, Birgitta Williams, Eleanor Stokes, Dietitians Ela Syzmula, Rhian Houghton, Alicja Lang, Hannah Gerard, Rachel Creighton, Physical Activity Specialists Tim Grove, Iain Waite, Andrew Kovelis, Neil Lockyer, Fay Tobby, Juliet Stevenson, Shauna Raugust, Lynne Smith, Anne Shelly, Lizzie Mason, Psychologists Dr Katie Murray and Dr Elizabeth Banwell, Administrators Catherine Altmeyer, Rosie Hooper, Vighnesh Seewoogoolam, Rubena Begum, Sam Dolbear, Glory Ayo. Mayden Health: Oliver Bateson, Chris May. Annie Holden (formerly of Mytime Active). Dr Adrian Bull, Former CEO Imperial College Health Partners. Imperial College Cardiovascular Academic Group – DW, CJ, KK, AA, JJ, Ms Annie Holden, Ms Agnieszka Adamska, PB.
References
Footnotes
Contributors SBC led all aspects of the manuscript, including statistical analyses, collation of results and manuscript preparation. KK contributed to the results interpretation and manuscript preparation. CJ led the design of the nursing intervention and also contributed to the manuscript. AA led the dietetic intervention and led on interpretation of the diet and anthropometrics data, as well as contribution to the manuscript. JJ led the physical activity intervention and collation of the physical-activity results and contributed to the mansucript. AB contributed to the manuscript and led on the public health aspect. BP was responsible for the statistical analyses. DW edited and revised the manuscript.
Funding The MyAction programme was funded by NHS Westminster and subsequently by Public Health, Westminster Council.
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.